> Seminar & Notice > Seminar
> Seminar & Notice > Seminar
| 제목 | Clinical Research : Osteoporosis (2) - Sep Oct 2000 | ||
|---|---|---|---|
| 작성자 | 관리자 | 조회수 | 4007 |
| 등록일 | 2004년 06월 12일 | ||
| 첨부파일 | |||
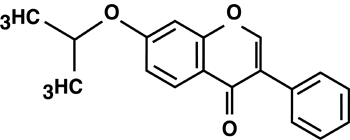
Molecular structure of Ipriflavone For additional information on ipriflavone, N-linked telopeptides and bone loss refer to the accompanying article entitled "Osteoporosis: A review focusing on ipriflavone and other key nutrients." Combine Ultra-Ostivone TM with our best calcium/ magnesium product Cal-6 + Mg.TM for maximum bone defense. Add our Ultra Preventive ® III multivitamin formula for the best in overall health maintenance and support. For additional information on our complete line of bone health formulations including ipriflavone-containing products as well as calcium/magnesium formulations, such as Calcium Microcrystalline Hydroxyapatite, refer to the latest Douglas Laboratories ® product catalog. If you would like a copy of the complete study on Ultra-Ostivone TM
Osteoporosis: A Review Focusing On Ipriflavone and Other Key Nutrients
Andrew Halpner, Ph.D.
Osteoporosis is a skeletal condition characterized by a decreased density of normally mineralized bone. This results in an increased risk of fracture, 1 and is a serious health issue facing older adults, especially postmenopausal woman. Approximately 30% of postmenopausal women in the United States have some degree of osteo-porosis present in the hip, spine, or forearm and are at risk for a fracture 2. By the age of 65, one third of women will experience a vertebral fracture and by extreme old age, one third of women will experience a hip fracture 3. However, unlike a fracture in a young individual, fractures in the elderly result in significant morbidity and mortality. Despite the fact that current methods of detection and treatment are improving, the diagnosis and initiation of treatment is often not initiated until the disease process has already taken a strong hold.
Risk Factors
Peak bone mass is reached between the ages of 25 - 30 years, and over a lifetime, a woman will lose about 50% of bone density at the spine and 30% at the hip. This loss can be exacerbated by either a decreased accumulation of bone during puberty, or an increased rate of loss later in life. Osteoporosis occurs more com-monly in Caucasians and Asian Americans than in African Americans 4. Certain medications such as steroids and gonadal hormone-releasing hormone agonists such as Lupron contribute to a loss of bone density by decreasing calcium absorption and increasing calcium loss from the body. For example, with only 7.5 mg prednisone/day bone loss has been observed in as little as 3 months 5. Excess thyroid hormone has also been shown to lead to osteoporosis in postmenopausal women not receiving estrogen. Specific risk factors for fracture include; poor balance, medications that cause drowsiness, family history of fracture, and a previous fracture.
Nutritional Treatment
Although calcium may be the most publicized nutrient effecting bone health, many other nutritional factors have now been implicated as having a role in maintaining bone structure and health. These factors appear to be essential for or complementary to the proper utilization of calcium, and include ipriflavone, vita-min D 3 , copper, zinc, manganese, silicon, vitamin K, and boron 6. Data are currently accumulating that demonstrate a beneficial effect of supplementation with certain nutrients on bone health.
Flavonoids (also known as bioflavonoids) are ubiquitous in plants that undergo photosynthesis. Scientists first become interested in flavonoids in the early 1930s when it was discovered that many of these compounds exhibited vitamin-like activity. Flavonoids have since been demon-strated to have antioxidant, antimicrobial, antimutagenic and anticarcinogenic activities 7. Recently, focus has centered on the effects that flavonoids may have on bone metabolism. Certain flavonoids, specifically a class of flavonoids called isoflavones, can exert estrogen-like activity. This has caused researchers to investigate their utility in preventing postmenopausal bone loss. While the data regarding the ability of isoflavones to help prevent bone loss are equivocal, ipriflavone (IP), a specific isoflavone derivative has received a significant amount of research with very positive results.
Ipriflavone is a non-hormonal agent currently used in many countries for the treatment of osteoporosis. Numerous well-controlled, clinical trials published in peer-reviewed journals have demonstrated IP's ability to slow the continual decline in bone mineral density commonly observed after menopause 8-14. Kovacs et al. 12 treated postmenopausal women with either IP, 600 mg/day or placebo for 1 year. After 6 months bone miner-al density (BMD) of the L2 - L4 vetebral region increased signifi-cantly in the IP-treated group and decreased in the placebo group. Gennari et al. |
|||